
In the week when the NHS celebrated its 75th birthday, there was an article in The Telegraph headlined ‘NHS to slash bureaucracy by recruiting doctors and nurses over pen-pushers’. This, of course, led to all the usual clichés about the NHS being full of managers.
I thought I’d take a look at what the evidence shows us on this subject.
What do NHS managers do?
A King’s Fund podcast in February 2023 looked at the subject of NHS managers. When asked to define the role, one manager said,
“We can one day be managing estates, we can one day be managing IT and information, we can one day be supporting clinical change in pathways and working with clinical teams, and equally we can be out there in the community.”
They described general managers and clinical operational managers, alongside finance, IT and HR managers:
“I think of that role as an enabler: what do you have to unblock today, to make tomorrow better, for your clinical staff and your patients; and that can be, often, estates, but it can be a whole mix of many things.”
“Managers have such a key role to play in staff wellbeing and that’s what I’m seeing, more and more, particularly after what we’ve been through, through COVID.”
“…How are we going to tackle this waiting list challenge? Who are the patient cohorts? What do you think about the urgency? How are we going to break this down? Give me some insight into what’s actually going on in operating theatre X or frustration area Y.”
The NHS needs people to oversee the waiting lists, assign the theatres for surgeries, organise the IT and infrastructure, deal with procurement, liaise with other organisations, and all those other jobs required to ensure the system runs properly.
Does the NHS have too many managers?
Work published in 2013 found that, if anything, the NHS was under-managed, with those who combined clinical and managerial roles outnumbering standalone managers four-to-one. These are doctors and nurses who are having to juggle their clinical work with managerial roles. Given the large clinical staff shortage we are currently facing, freeing up our doctors and nurses to treat patients by bringing in more dedicated managers, would seem like a sensible idea.
Managers in the NHS currently make up only two per cent of the entire workforce. This compares to 9.5 per cent of the UK workforce as a whole being made up of ‘managers, directors and senior officials’.
The first of these charts is 10 years old, and the second shows that management positions as a proportion of the workforce have fallen since then, but they highlight the make-up of the NHS by staff type.
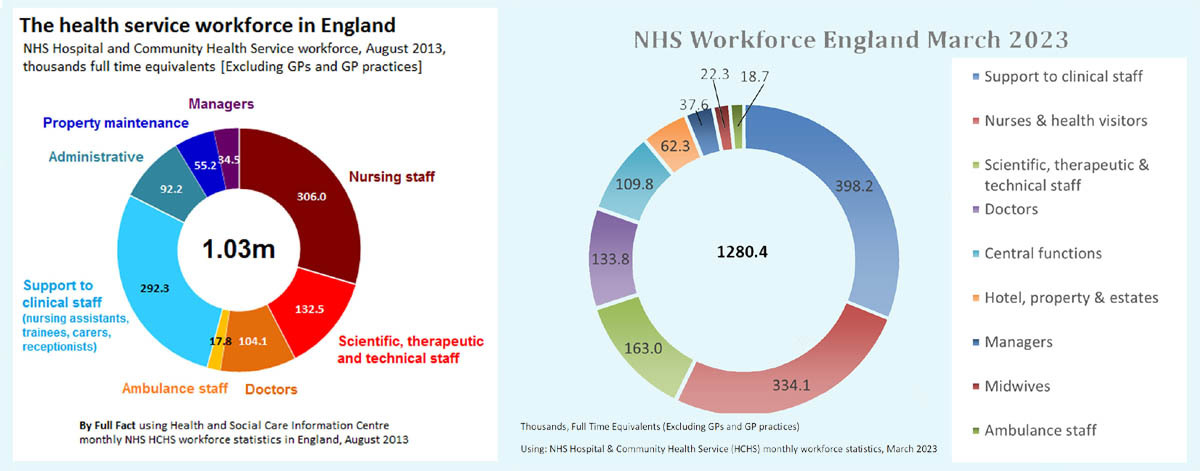
Management roles within the NHS having been cut following the Lansley Reforms in 2010, a freedom of information request in 2014 highlighted that the NHS was spending £640m per year bringing consultants in to perform managerial roles. As ever, private firms are profiting off the back of cuts made to the NHS. This seems to highlight further that, rather than containing too MANY managers, the NHS has far too FEW.
Are NHS managers overpaid?
The NHS is one of the most complex organisations in the world. It is not only the largest employer in the UK, but the largest employer in the whole of Europe. It currently sits as the seventh largest employer worldwide.
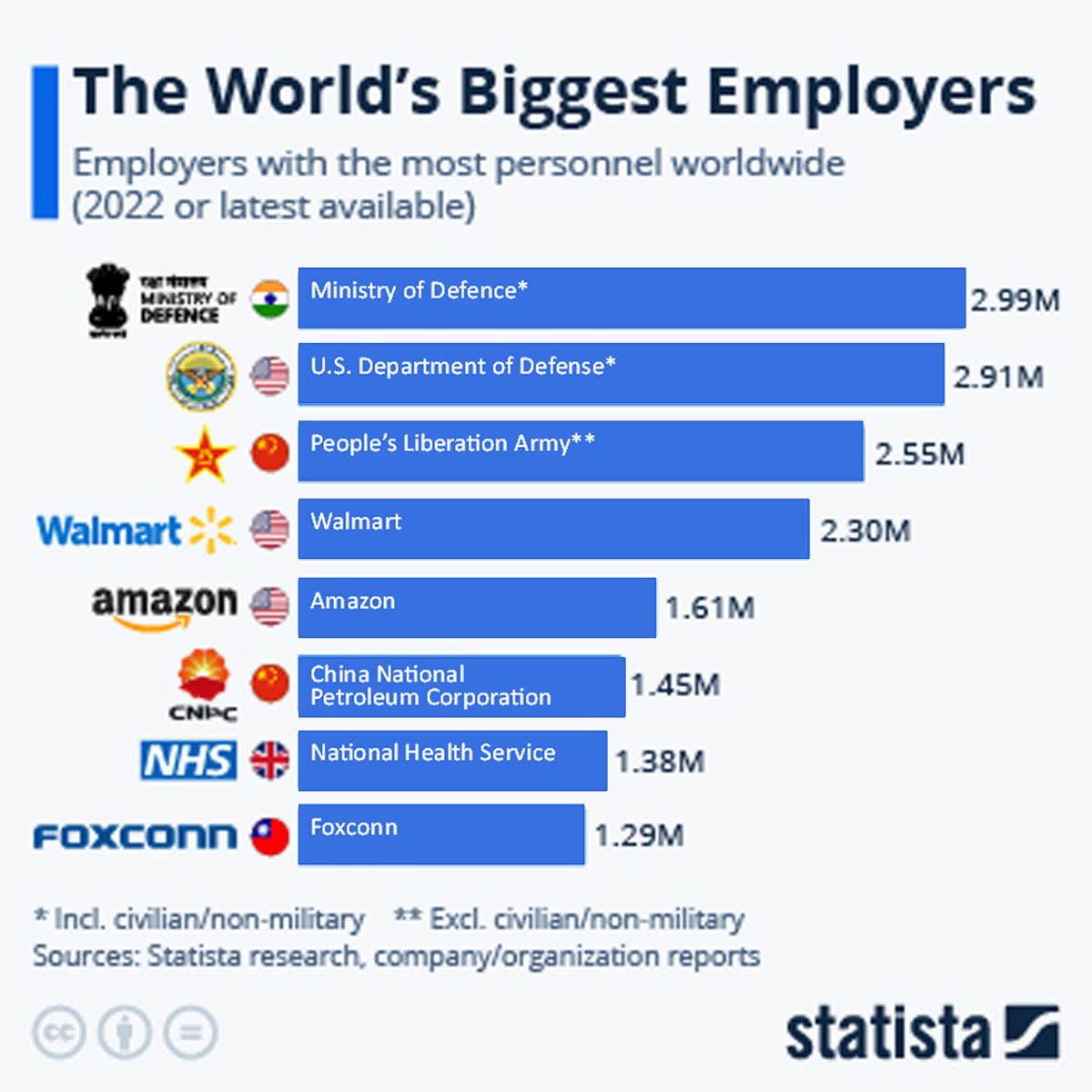
Despite the size and complexity of the NHS, most NHS Trust chief executives are paid between £200,000 and £250,000. The chief executive of NHS England and NHS Improvement, who is responsible for the NHS’s annual budget of almost £150bn and the service’s 1.38m staff, is paid around £200,000.
Compare this to the Chief Executive of Thames Water (which has a revenue of £2bn and 7000 staff) who gets paid £2,000,000 per year plus bonuses.
I think it is safe to say that NHS managers are far from being overpaid!
Is the NHS bureaucratically inefficient?
On measures of efficiency such as administrative spending as a proportion of total spend, the NHS ranks well against other countries. And out of 11 comparator healthcare systems, the NHS ranks fourth for administrative efficiency.
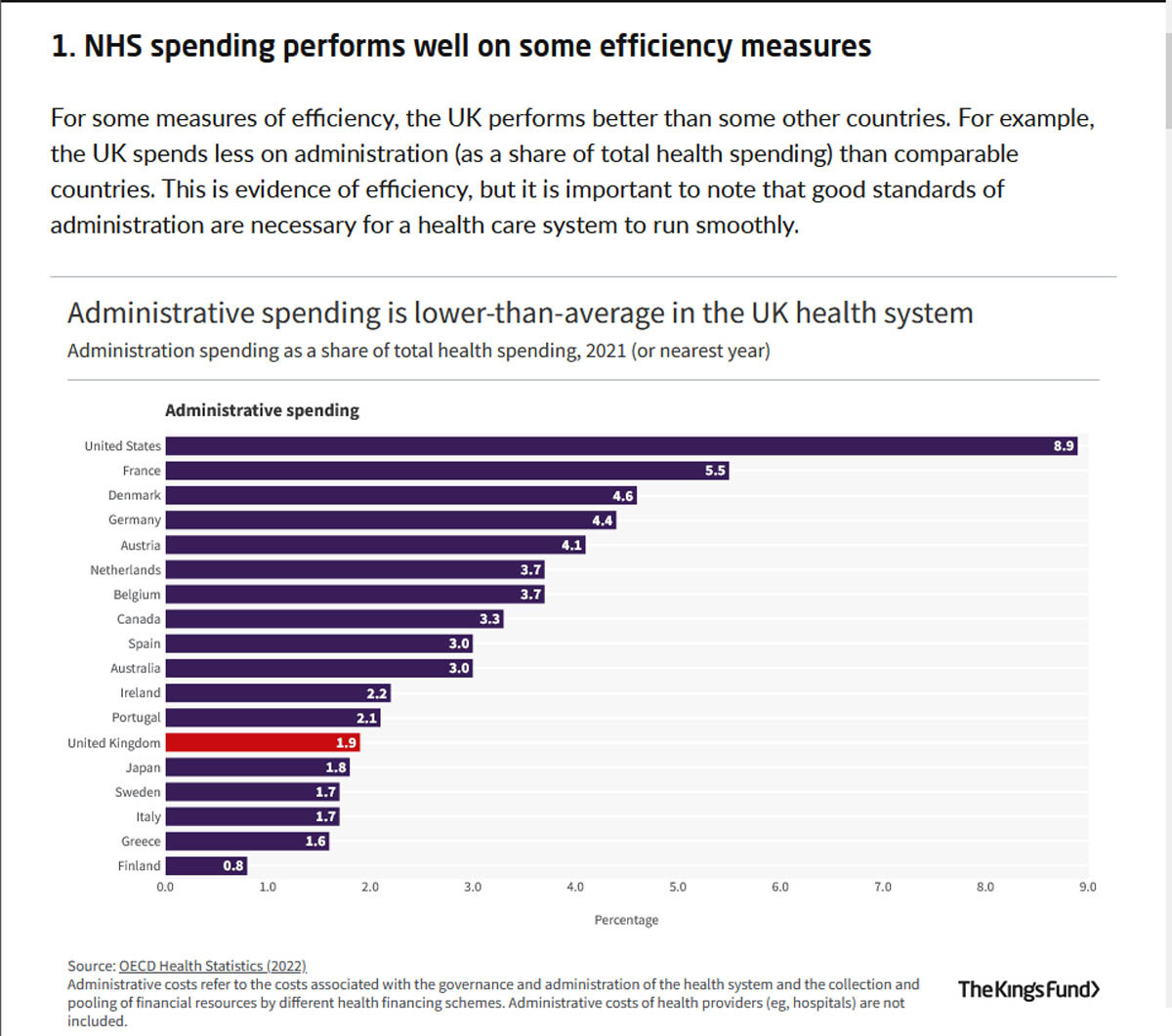
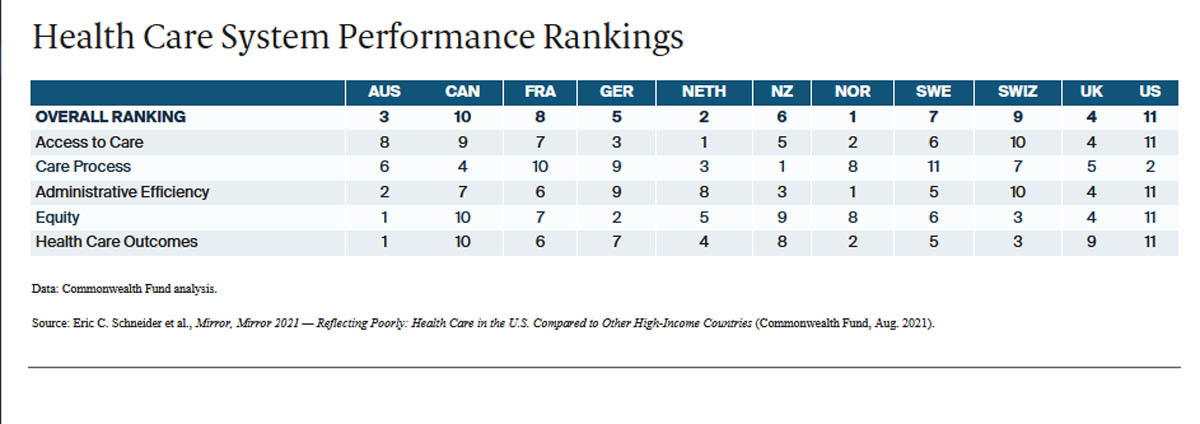
None of this would suggest that the NHS is being run inefficiently. Obviously, there are always improvements that can be made, but the strategic planning and implementing of those kinds of reforms require MANAGERS to plan and oversee them. Getting an already overstretched clinical workforce to make more ‘efficiency savings’ by getting rid of managerial roles seems to be a grossly unthought-through plan.
The managers within the NHS do an absolutely vital role in delivering your care, and they do it in circumstances that managers in other industries couldn’t begin to imagine. They manage and run the seventh largest organisation on the planet, and they achieve it efficiently despite comprising only two per cent of the organisation.
Reducing managers isn’t going to reduce ‘bureaucracy’, as The Telegraph suggested. It would simply make the organisation function more poorly, and take clinical staff away from their clinical work – which is caring for patients and their loved ones.
I’ll end on this comment by NHS Doctor, Dr Newbould:
“To me the fact that we do now have managers has completely revolutionised our work. Before, consultants would have to spend many hours doing admin, drafting safety policies, and doing document management. Now we have professionals specifically doing this. Even audit is managed by a professional person (we have to do the audit ourselves of course!) but the documentation etc is managed by someone who does that as their job. It’s revolutionary! Makes life so much easier.”




